Negative
Cells obtained appear normal or there is no identifiable infection.

L-SIL
Low Grade Squamous Intraepithelial Lesion.
It is a lesion not invasive of the epithelium that covers the cervix associated, in the majority of cases, with a transient infection by HPV (Human Papilloma Virus).
The term "low grade" identifies a minor modifications in the morphology of squamous cell epithelial. The confirmation of the real presence of alterations and the secure identification of the type of alteration is supplied solely by the execution of further investigations as the colposcopic examination and the possible subsequent biopsy; the histological examination carried out on the latter can confirm whether or not the outcome of the Pap test. Usually a L-SIL in cervical cytology is histologically a mild dysplasia or CIN I.
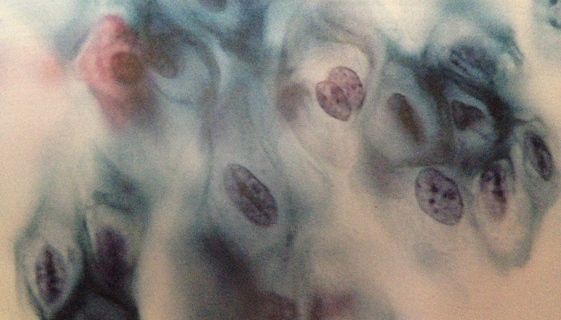
H-SIL
High Grade Squamous Intraepithelial Lesion.
It refers to anomalies in the morphology of the cells more marked and significant compared to the L-SIL.
Also in this case the cells affected are those of the outer covering of the neck of the womb and, as for the injury of low degree, the later indication is the colposcopy.
The H-SIL in histology correspond to moderate/severe dysplasia (CIN II, CIN III).
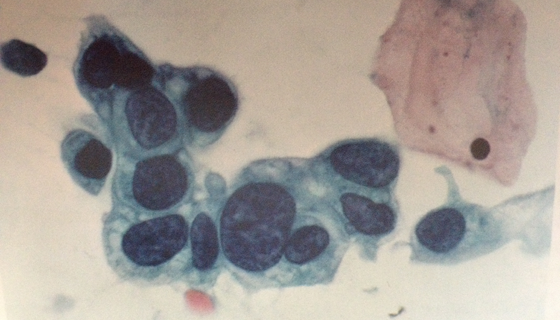
AIS
Adenocarcinoma in situ.
It is a endocervical glandular lesion of high degree in the absence of infiltration; this definition indicates that have been identified severe changes in the morphology of glandular cells surface lining the endocervical canal.
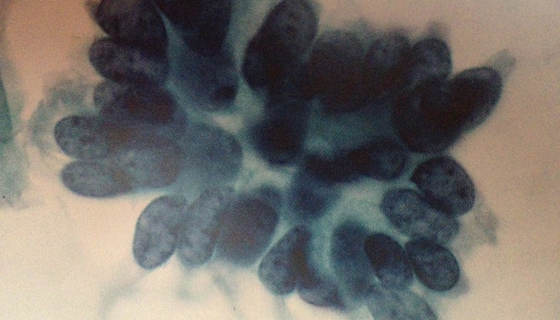
Carcinoma
Squamous cell carcinoma cells.
Malignant neoplasia with invasive differentiation squamous cell. With this definition you indicate severe changes in the squamous cells of the surface of the uterine cervix.
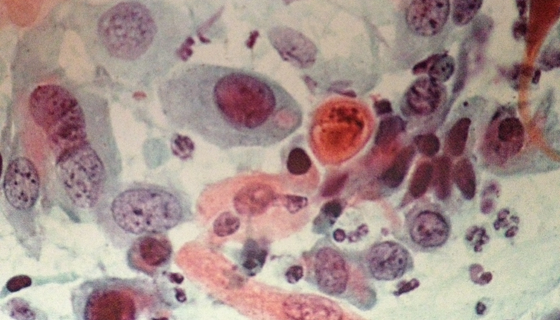
ASC-US
Atypical squamous cells of undetermined significance.
The term refers to cytological abnormalities suggestive of squamous intraepithelial lesion, qualitatively or quantitatively insufficient for a definitive interpretation.
Sometimes these changes are related to HPV infection; in other cases, on the other hand, there are a few conditions not pathological that can produce cytological modifications of undetermined significance as the inflammation, atrophy, infections or micetali artifacts related to the preparation of the sample under examination.
In any case, the next instruction is the repetition of the examination after a few months, the repetition after therapy or the execution of the HPV Test.
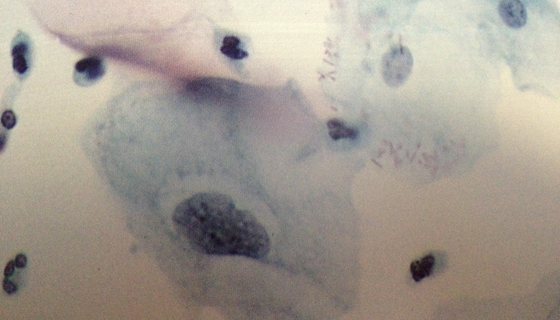
ASC-H
Atypical squamous cells - cannot exclude HSIL.
In this case, the next instruction is to sending the patient in colposcopy because the alterations i quote-morphological highlighted are strongly suggestive of the presence of a lesion of high degree. We remember that, as for ASC- US, there are a number of conditions that are not pathological conditions that may mimic a H-SIL, without necessarily be; The squamous metaplasia immature for example, a atrophic vaginitis or still endometrial regressive cells.
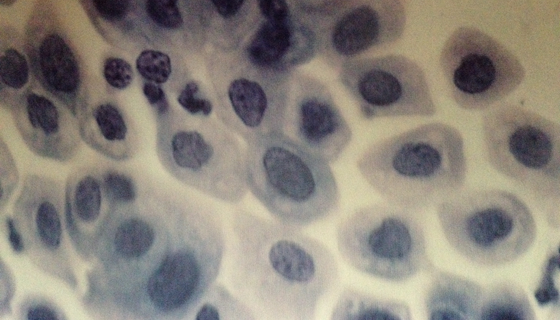
AGC
Atypical Glandular Cells not otherwise specified.
For this cytological category a premise is needed: the cervical cytology (pap test) is a screening test for the intraepithelial squamous lesions and squamous cell carcinoma. It cannot be considered a highly reliable test for the diagnosis of lesions in the endocervice and even less to the endometrium because its sensitivity is limited to problems in both sampling and interpretation.
However when you are unable to identify the cytological atypia glandular, these lesions should be reported with reference to the type of cellular origin (endocervical or endometrial); this differentiation will be useful for subsequent clinical investigations.
Where this is not possible, we use the terminology of generic "glandular cells Atypical- not otherwise specified" (AGC-NAS).
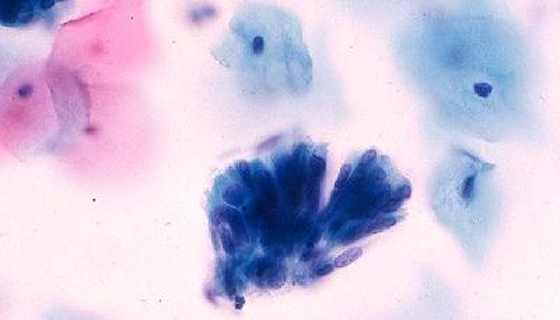
Adenocarcinoma
Endocervical, endometrial, extrauterine or not otherwise specified.
Can be of type endocervical if it is assumed that the cells affected originate from endocervical canal, endometrial type if it is assumed that the origin is the endometrium or type extrauterino (ovarian origin or, less frequently, extrauterine).
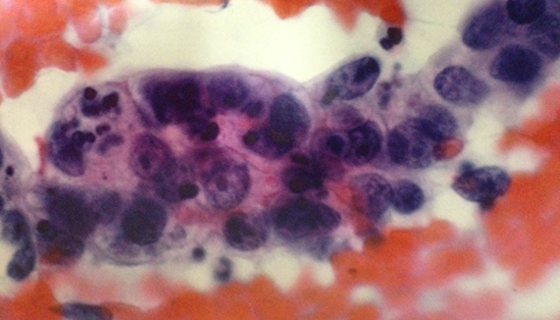
CTM
Malignant cells not otherwise specified.
They are cells that give rise to malignant tumors, i.e. tissues that grow in excess and in an uncoordinated way with respect to the normal ones. Cells are unable to control their proliferation and may invade other organs even distant.
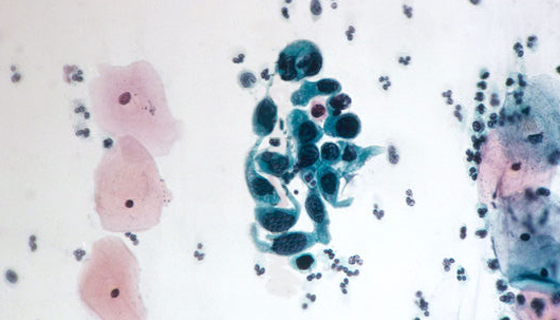
Warnings:
It is necessary to know that the Pap Test (Pap Smear) provides important information on the state of health of the neck of the uterus (cervix); to ensure the integrity of the entire genital apparatus as a result of any gynecological disorders and necessary to undergo periodically to a gynecological examination specialist.
Who should perform the examination?
According to European guidelines for the age group between 25 and 65 years would be appropriate to conduct the test at least every three years.
In the United States is run every 12 months from the age of 21. All data provided are for information purposes. For further information consult a physician.
We disclaim any responsibility for any damage to people.
The Human Papillomavirus are DNA viruses that are transmitted sexually and that replicate in the epithelial cells. Today there is evidence of the presence of HPV infection in about 95% of cervical carcinomas.
They have been identified over 150 types of HPV of which about 40 are considered to be a non-oncogenes, cause i.e. simply anogenital warts- genitals.
Therefore, there is a major subdivision in the great family of HPV between types (genotypes) at high risk (HR) to produce neoplasia (and its precursors) genotypes and low-risk (LR) neoplastic development.
By way of example:
- (some) Genoitpi high risk (HPV-HR): 16, 18, 31, 33, 35, 39, 45, 51, 52, 56,...
- (some) genotypes as low risk HPV-LR): 6, 11, 42, 43, 44,...
In the presence of an abnormal Pap smear and/or under indication of your gynecologist is useful to undergo HPV Test, which is more in order to set an appropriate therapeutic program and surveillance.
There are different methods of investigation of laboratory that have substantially with the aim to identify the presence of the virus in the cells of the uterine cervix and to discriminate between the different genotypes.
It may be that it is infected with one or more genotypes with high and low risk or both; Most of the infections and transient because the virus is eliminated by the immune system before being able to develop a pathogenic effect. In the case of persistent infection the time between the infection and the onset of cancerous lesions (L-SIL/H-SIL) is about 3-5 years, while the latency for the onset of cervical carcinoma can be over 10 years.
It is absolutely necessary to remember that this is the only test that can confirm the presence/absence of the virus; a negative Pap test may not give the certainty of not be infected since it is able to detect only the presence of HPV 'active' and not latent.